
After COVID-19, the hunt for the next 'Disease X' continuesBCCL
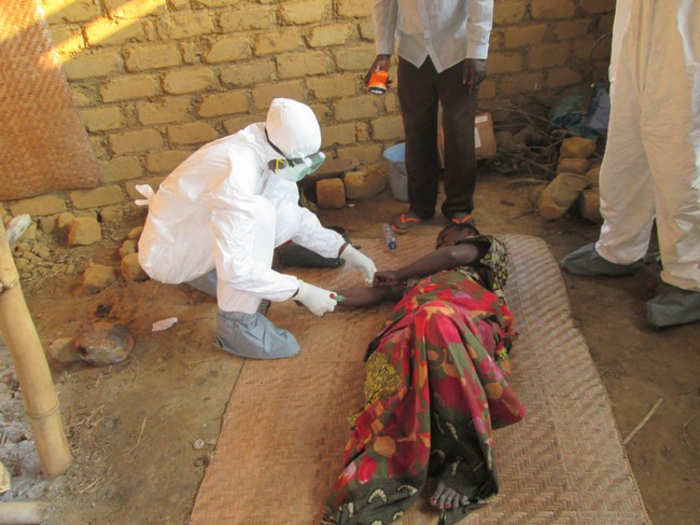
The first Ebola vaccine was only approved in January 2020. That’s six years after the Ebola pandemic struck West Africa, killing over 11,000 people. The ongoing outbreak in the Democratic Republic of Congo has reported 3,456 cases so far and 2,276 deaths.
Ebola proliferates quickly and is one of the deadliest diseases on the planet. It needs close human contact to spread, often through bodily fluids like blood, faeces, and vomit. The transmission method put not only the patient’s contacts at risk but also the associate healthcare workers.

The Marburg Virus Disease is a cousin of the Ebola virus. It spreads in a similar way, causes the same symptoms, and even touching a deceased patient can result in transmission.
The only difference is that Marburg is deadlier, with a fatality rate hitting 88%. However, the silver lining is that it has so far been stopped in its tracks.
The most recent outbreak, which occurred in Uganda, infected three people — all of whom died. The previous outbreak in 2005 resulted in over 200 infections in Angola, 90% of whom died.

Lassa Fever is a viral haemorrhagic illness that damages organs and ruptures blood vessels. According to GAVI, every one in five people infected with the Lassa virus has severe disease affecting the liver, spleen, or kidneys.
It is often transmitted by the urine or faeces of Mastomys rats, which are native to Africa, via contaminated household objects. Once the infection jumps from animal to human, it can further be transmitted to other humans who may come in contact with the blood or organ tissue of a patient.
Even after recovery, a Lassa fever infection can result in long-term hearing loss.
While Ebola and Marburg cause sporadic and deadly outbreaks and then subside, Lassa fever occurs more regularly and sticks around for longer. In several West African countries, where outbreaks have occurred, the infection has killed between 1% to 15% of those infected.
Due to the limited amount of surveillance and little evidence about deaths in the region, there is no exact tally of how many lives the virus has claimed so far. Experts estimate there are between 100,000 and 300,000 infections of Lassa fever annually, with around 5,000 deaths overall.

This virus has only emerged over the last two decades. Since it is a viral respiratory illness, doctors believe that it spreads through respiratory secretions such as coughing. However, this has not yet been proven.
Thus far, MERS-CoV isn’t known for spreading easily from person to person unless there is close contact.
It was first spotted in Saudi Arabia in 2012. Since then, sporadic outbreaks are estimated to have caused 2,519 cases and 866 deaths.

SARS has already been at the heart of one pandemic back in 2003 when it infected over 8,000 people and killed 775 across 37 countries.
It may look paltry in front of the damage done by COVID-19, but it was a goliath in its day. And, there isn’t any guarantee that it won’t make a deadlier comeback.

The NIPAH virus is a distant cousin of the measles virus. It first emerged in 1998 and has been spotted frequently since in South-East Asia.
Symptoms of the virus include extreme headaches, a stiff neck, vomiting, dizziness and falling into a coma — all indications of brain swelling.
Nipah is common in bats, specifically fruit bats in South-East Asia. It spreads through close contact with infected pigs and raw food contaminated with urine or saliva from infected bats.
It can also be transmitted through coughing and sneezing. However, the primary concern is what may happen if the virus mutates, giving it the ability to spread quickly.
The most recent 2018 outbreaks in Kerala were contained well, which has been attributed to the state’s relatively robust health infrastructure. There were a total of 23 cases and 17 deaths.

The ZIKA virus isn’t the deadliest of the viruses on this list. Usually it causes mild symptoms like fever, rash, and muscle pain.
However, between 2015 and 2016, the virus caused birth defects, which were dubbed as the ‘congenital Zika syndrome’. There is a higher risk of miscarriage, and babies born to pregnant women infected with Zika are at risk of microcephaly.
In that one year, more than 500,000 cases of ZIKA were reported, resulting in 18 deaths and 3,700 babies born with birth defects.
Scientists have also found that babies previously born with no visible symptoms of the ZIKA virus could exhibit problems such as vision loss later in infancy.
The virus is spread by Aedes mosquitoes, which also transmit dengue and chikungunya viruses.

The Crimean-Congo haemorrhagic fever is mostly restricted to animals spread through tick bites. However, humans can catch it too if they come in contact with a recently slaughtered animal that was infected.
Although rare, there has been human-to-human transmission through exposure to bodily fluids of infected people.
Initially, the virus causes flu-like symptoms. Some cases may also experience light sensitivity or stiffness of the neck that could be confused with measles.
However, if not caught early enough, the Crimean-Congo haemorrhagic fever can result in severe and uncontrollable bleeding.
Crimean-Congo haemorrhagic fever is not a pandemic yet, but it is already endemic in many countries in Asia, Africa, and the Balkans, which are home to the disease-spreading tick species.
As recently as 2018, there were 483 cases of the Crimean-Congo haemorrhagic fever in Afghanistan and 59 deaths.

Like the Crimean-Congo haemorrhagic fever, Rift Valley fever is also known to restrict itself to animals. Instead of ticks, it's mosquitos that carry the disease.
Nonetheless, people can still get infected if they come into contact with the bodily fluids — such as blood or milk — of an infected animal. Or if one of the carrier mosquitos bites them.
The good news is that no case of human-to-human transmission has been reported thus far.
When a human does get infected, they are likely to exhibit fever and muscle aches initially. As the infection gets more severe, it can cause blindness, swelling of the brain, or uncontrollable bleeding.
Several countries in Africa have reported outbreaks for decades. But, since 2000, Rift Valley fever outbreaks have also been spotted in the Middle East.

Smallpox may have been eradicated from the face of the planet, but it has a cousin that still poses a threat called Monkeypox.
It is mostly spread by contact with wild animals such as rodents and primates. However, it can also spread between people through contact with lesions, body fluids, respiratory droplets, or contaminated clothes or bedding.
The virus’ symptoms are also similar to smallpox with a widespread pustular rash with fever and exhaustion.
The vaccinia vaccine, which was used to eradicate smallpox, can also protect against monkeypox. A new third-generation vaccinia vaccine has already been approved for the prevention of monkeypox.
But, travel and trade in pets have caused monkeypox to spread across the globe — from Central and West Africa to North America and European countries such as the UK. Luckily, all resulting outbreaks have been brought under control so far.
 Global stocks rally even as Sensex, Nifty fall sharply on Friday
Global stocks rally even as Sensex, Nifty fall sharply on Friday
 In second consecutive week of decline, forex kitty drops $2.28 bn to $640.33 bn
In second consecutive week of decline, forex kitty drops $2.28 bn to $640.33 bn
 SBI Life Q4 profit rises 4% to ₹811 crore
SBI Life Q4 profit rises 4% to ₹811 crore

Copyright © 2024. Times Internet Limited. All rights reserved.For reprint rights. Times Syndication Service.